Using evidence-based best practices to create great breast augmentation outcomes
Patients often ask me what type of incision is best for placing their implants, or if they will get antibiotics after surgery. For these questions and many others, in today’s world of modern medicine it is now possible to give definitive answers that are evidence-based, not just based on a hunch or a pattern of practice. This approach to decision making is a critical part of the best practice of medicine – especially when it comes to the art and science of breast augmentation, yes even right here in Columbus!
What incision type is best for placing breast implants?
Based on mountains of evidence, this question can be answered with confidence – and the answer based on that evidence is the inframammary incision. This implant-placement approach has been shown in many studies to lower the risk of infection, as well as reducing certain other complications. The inframammary incision also has the added benefits of applying less physical strain to the implant as it is being placed, as well as providing a good “hiding spot” for the incision scar in the breast fold (vs. a periareolar incision). The inframammary incision has been my “go-to” for primary breast augmentations from the beginning of my practice in 1996. As to my own cohort of primary breast augmentation patients, this incision placement has had a consistently low complication rate.
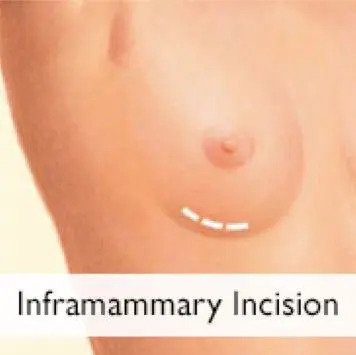
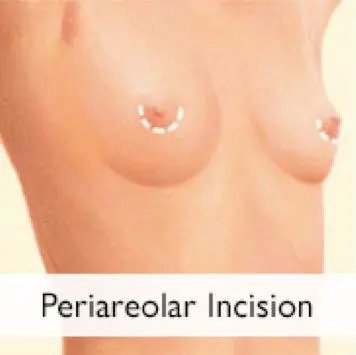
Will I need antibiotics after breast augmentation surgery?
When it comes to infection after a breast augmentation, nothing could be worse. Therefore, historically many plastic surgeons here in Columbus and around the world have given patients oral antibiotics for a short period after. This may seem like a reasonable practice; however, here again there is plenty of data that shows a single pre-operative dose of IV antibiotics is adequate to prevent infection. And as you may have heard, adding post-op antibiotics risks increasing the number of antibiotic-resistant bacteria, which would make the world a more dangerous place for us all. For this reason, approximately 15 years ago I eliminated post-op antibiotics for breast augmentation patients, and crucially over this period of time I have not had a single breast augmentation patient experience an infection.
“Knock on wood?” I think not. As physicians we are trained to evaluate all available data, and act in the way that promotes both patent safety and optimal outcomes. Everybody benefits when we adhere to best practices that are backed up with real evidence, and you can believe that in the future continuing research will continue to improve results.


If a person is allergic to Keflex and does not want CIPRO due to well documented adverse side-effects, what other IV prophylactic antibiotics are good to consider, but that are also not overly strong “nuclear options” for breast explant en bloc surgery? Thanks!